An Atlas of Lumps and Bumps, Part 37: Keratosis Pilaris
Keratosis Pilaris
Keratosis pilaris, frequently referred to as “chicken skin” by patients, is a disorder of keratinization of the infundibulum of pilosebaceous follicles characterized by keratinous plugs in the follicular orifices with varying degrees of perifollicular erythema.1-7 Keratosis pilaris develops during childhood and reaches its peak during adolescence. The prevalence in adolescents of both genders is estimated to be at least 50%, while up to 80% of adolescent girls may be affected.8-10 The disorder involutes spontaneously and is less common during adult life.5,9 There is no racial predominance.11,12
The exact etiology is not known. A defect in the keratinization process resulting in follicular plugging may be responsible.13 Mutations in the filaggrin gene may result in proliferation and inflammation of keratinocytes.13 Mutations of the ATP-binding cassette sub-family A member 12 (ABCA12) gene may account for some of the cases.14 An autosomal dominant mode of inheritance with variable penetrance has been postulated.8,9,11 The high prevalence and intensity seen at puberty suggests a hormonal influence. Hyperandrogenism in the presence of obesity is associated with an increased incidence and severity of keratosis pilaris.5
Keratosis pilaris is more common in patients with ichthyosis vulgaris, atopic dermatitis, and ectodermal dysplasia.7,8,15 Keratosis pilaris has also been reported to occur following the use of certain medications (e.g., nilotinib, vemurafenib) or as a reaction to contact with cutting oil.16-20
Other conditions associated with keratosis pilaris include Noonan syndrome, Down syndrome, Cushing disease, diabetes mellitus, hypothyroidism, vitamin A intoxication, vitamin C deficiency, malnutrition, monilethrix, Hodgkin disease, monosomy 18p, and cardio-facio-cutaneous syndrome.8,11,15,21-24 Given the high prevalence of keratosis pilaris, caution is suggested in the interpretation of these associations.8
Keratosis pilaris typically presents as asymptomatic, minute, discrete, keratotic, follicular papules with variable perifollicular erythema (Figure 1).9
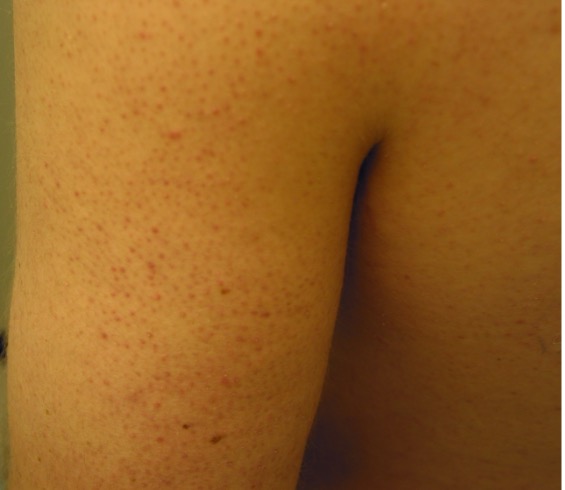
Fig. 1. Keratosis pilaris typically presents as asymptomatic, minute, discrete, keratotic, follicular papules with variable perifollicular erythema.
The lesions are not grouped and show no tendency to coalesce to form plaques.1-4 The affected skin looks like gooseflesh and feels like sandpaper.1-4 Keratin plugs cannot be expressed with pressure.8 The lesions are usually bilateral and symmetrical.1-4 Sites of predilection include the lateral aspects of the upper arms, most commonly, followed by the thighs and face (Figure 2).1-4

Fig. 2. Sites of predilection include the lateral aspects of the upper arms, most commonly, followed by the thighs and face.
The trunk buttocks, and distal extremities may also be affected.15 The hands and feet are usually spared, but palmoplantar markings are more accentuated.1-4
Several clinical variants have been recognized, namely, unilateral keratosis pilaris, keratosis pilaris rubra, erythromelanosis follicularis faciei et colli, keratosis pilaris atrophicans, and papular, profuse, and precocious keratosis pilaris (with an age of onset younger than 18 months of age).10,13,25-30
The diagnosis of keratosis pilaris is mainly clinical based on the presence of rough papules with follicular involvement mainly on the extensor surfaces of the upper arms, and less commonly, the thighs. The clinical features are so distinct that the diagnosis is usually straightforward. Typical dermoscopic features include coiled or twisted vellus hairs surrounded by peripilar casts within the stratum corneum.6,15,31 Other features include perifollicular erythema/hyperpigmentation and scaling.6,15,31
Keratosis pilaris can be cosmetically unsightly. The rough skin texture can lead to psychosocial impact in affected patients.13
AFFILIATIONS:
1Clinical Professor of Pediatrics, the University of Calgary, Calgary, Alberta, Canada
2Pediatric Consultant, the Alberta Children’s Hospital, Calgary, Alberta, Canada
3Dermatologist, Medical Director and Founder, the Toronto Dermatology Centre, Toronto, Ontario, Canada
4Associate Clinical Professor of Pediatrics, Dermatology and Skin Sciences, the University of British Columbia, Vancouver, British Columbia, Canada.
5Pediatric Dermatologist, the Pediatric Institute, Kuala Lumpur General Hospital, Kuala Lumpur, Malaysia
CITATION:
Leung AKC, Barankin B, Lam JM, Leong KF. An atlas of lumps and bumps, part 37: keratosis pilaris. Consultant. 2024;64(3):e3. doi:10.25270/con.2024.03.000001
CORRESPONDENCE:
Alexander K. C. Leung, MD, #200, 233 16th Ave NW, Calgary, AB T2M 0H5, Canada (aleung@ucalgary.ca)
EDITOR’S NOTE:
This article is part of a series describing and differentiating dermatologic lumps and bumps. To access previously published articles in the series, visit: https://www.consultant360.com/resource-center/atlas-lumps-and-bumps.
REFERENCES
- Leung AKC, Kao CP. Keratosis pilaris. Consultant for Pediatricians. 2010;9:197-198.
- Leung AKC, Robson WL. Keratosis pilaris. In: Lang F, ed. The Encyclopedia of Molecular Mechanisms of Disease. Berlin: Springer-Verlag, 2009, pp1119-1120.
- Leung AKC. Keratosis pilaris. In: Leung AKC, ed. Common Problems in Ambulatory Pediatrics: Specific Clinical Problems, volume 2. New York: Nova Science Publishers, Inc., 2011; 239-242.
- Leung AKC, Barankin B. Keratosis pilaris. Austin J Pediatr. 2014;1(1):2.
- Barth JH, Wojnarowska F, Dawber RP. Is keratosis pilaris another androgen-dependent dermatosis? Clin Exp Dermatol. 1988;13(4):240-241. doi: 10.1111/j.1365-2230.1988.tb00688.x.
- Ismail S, Omar SS. Clinical and dermoscopic evaluation of fractional carbon dioxide laser in management of keratosis pilaris in Egyptian type skin. J Cosmet Dermatol. 2020;19(5):1110-1120. doi: 10.1111/jocd.13140.
- Thomas M, Khopkar US. Keratosis pilaris revisited: is it more than just a follicular keratosis? Int J Trichology. 2012;4(4):255-258. doi: 10.4103/0974-7753.111215.
- Lateef A, Schwartz RA, Janniger CK. Keratosis pilaris. Cutis. 1999;63(4):205-207.
- Poskitt L, Wilkinson JD. Natural history of keratosis pilaris. Br J Dermatol. 1994;130(6):711-713. doi: 10.1111/j.1365-2133.1994.tb03406.x.
- Sobhi RM, Adawy NAH, Zaky IS. "Comparative study between the efficacy of fractional CO2 laser, Q-switched Nd:YAG laser (1064 nm), and both types in treatment of keratosis pilaris". Lasers Med Sci. 2020;35(6):1367-1376. doi: 10.1007/s10103-020-02956-w.
- Garwood JD. Keratosis pilaris. Am Fam Physician. 1978;17(2):151-152.
- Novick N. Practical management of widespread, atypical keratosis pilaris. J Am Acad Dermatol. 1984;11(2 Pt 1):305-306. doi: 10.1016/s0190-9622(84)80522-8.
- Maghfour J, Ly S, Haidari W, Taylor SL, Feldman SR. Treatment of keratosis pilaris and its variants: a systematic review. J Dermatolog Treat. 2020:1-12. doi: 10.1080/09546634.2020.1818678.
- Liu F, Yang Y, Zheng Y, Liang YH, Zeng K. Mutation and expression of ABCA12 in keratosis pilaris and nevus comedonicus. Mol Med Rep. 2018;18(3):3153-3158. doi: 10.3892/mmr.2018.9342.
- Pennycook KB, McCready TA. Keratosis pilaris. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan–2020 Jun 29. PMID: 31536314.
- Georgouras K. Oil contact keratosis pilaris. Australas J Dermatol. 1985;26(3):108-112. doi: 10.1111/j.1440-0960.1985.tb01760.x.
- Jimenez-Cauhe J, Fernandez-Gonzalez P, Ortega-Quijano D, Fernandez-Nieto D, Saceda-Corralo D. Keratosis pilaris-like eruption induced by nilotinib. G Ital Dermatol Venereol. 2019 Jul 12. doi: 10.23736/S0392-0488.19.06333-8.
- Khetarpal S, Sood A, Billings SD. Nilontinib induced keratosis pilaris atrophicans. Dermatol Online J. 2016;22(8):13030/qt2rx3z0m4.
- Oro-Ayude M, Feito M, Quintana-Castanedo L, Beato-Merino MJ, De Lucas R. Keratosis pilaris-like eruption secondary to nilotinib in a child. Pediatr Dermatol. 2020;37(5):968-969. doi: 10.1111/pde.14267.
- Wang CM, Fleming KF, Hsu S. A case of vemurafenib-induced keratosis pilaris-like eruption. Dermatol Online J. 2012;18(4):7. PMID: 22559022.
- Fernández-Canga P, Vázquez-Osorio I, Álvarez-Cuesta CC, Rodríguez-Díaz E. Noonan syndrome with multiple lentigines and prominent keratosis pilaris. J Dtsch Dermatol Ges. 2019;17(7):749-751. doi: 10.1111/ddg.13880.
- Purnak S, Topçu V, Çavdarlı B, Kadan E, Yalçın B. Widespread keratosis pilaris in a patient with Noonan syndrome with multiple lentigines. Int J Dermatol. 2018 ;57(11):e140-e141. doi: 10.1111/ijd.14209.
- Thomsen K, Nyfors A. Keratosis pilaris: skin marker of Hodgkin disease? Arch Dermatol. 1973;107(4):629-630. PMID: 4697700.
- Zouboulis CC, Stratakis CA, Rinck G, et al. Ulerythema ophryogenes and keratosis pilaris in a child with monosomy 18p. Pediatr Dermatol. 1994;11(2):172-175. doi: 10.1111/j.1525-1470.1994.tb00575.x.
- Al Hawsawi K, Aljuhani O, Niaz G, Fallatah H, Alhawsawi A. Erythromelanosis follicularis faciei: A case report and review of the literature. Case Rep Dermatol. 2015;7(3):335-339. doi: 10.1159/000442343.
- Castela E, Chiaverini C, Boralevi F, Hugues R, Lacour JP. Papular, profuse, and precocious keratosis pilaris. Pediatr Dermatol. 2012 May-Jun;29(3):285-8. doi: 10.1111/j.1525-1470.2011.01616.x.
- Ma H, Xu Q, Zhu G, Su X, Yin S, Lu C, Lai W. Unilateral keratosis pilaris occurring on linear hypopigmentation patches: a new variant of keratosis pilaris in an Asian? J Dermatol. 2015;42(4):437-8. doi: 10.1111/1346-8138.12821.
- Rather S, Yaseen A, Mukhija M. Erythromelanosis follicularis faciei et colli - A cross-sectional, descriptive study. Indian J Dermatol. 2016 May-Jun;61(3):308-13. doi: 10.4103/0019-5154.182419.
- Volks N, Fölster-Holst R. Erythromelanosis follicularis faciei--a variant of keratosis pilaris? J Dtsch Dermatol Ges. 2015;13(1):51-54. doi: 10.1111/ddg.12457.
- Zhu JW, Lu ZF, Zheng M. Unilateral generalized keratosis pilaris following pregnancy. Cutis. 2014;94(4):203-205.
- Sonthalia S, Bhatia J, Thomas M. Dermoscopy of keratosis pilaris. Indian Dermatol Online J. 2019;10(5):613-614. doi: 10.4103/idoj.IDOJ_279_18.


