Peer Reviewed
An Atlas of Lumps and Bumps: Part 26
AFFILIATIONS:
1Clinical Professor of Pediatrics, the University of Calgary
2Pediatric Consultant, the Alberta Children’s Hospital, Calgary, Alberta, Canada
3Dermatologist, Medical Director and Founder, the Toronto Dermatology Centre, Toronto, Ontario, Canada
4Associate Clinical Professor of Pediatrics, Dermatology and Skin Sciences, the University of British Columbia, Vancouver, British Columbia, Canada
5Pediatric Dermatologist, the Pediatric Institute, Kuala Lumpur General Hospital, Kuala Lumpur, Malaysia
CITATION:
Leung AKC, Barankin B, Lam JM, Leong KF. An atlas of lumps and bumps, part 26. Consultant. 2023;63(4):e10. doi:10.25270/con.2023.04.000001.
DISCLOSURES:
Dr Leung is the series editor. He was not involved with the handling of this paper, which was sent out for independent external peer review.
CORRESPONDENCE:
Alexander K. C. Leung, MD, #200, 233 16th Ave NW, Calgary, AB T2M 0H5, Canada (aleung@ucalgary.ca)
EDITOR’S NOTE:
This article is part of a series describing and differentiating dermatologic lumps and bumps. To access previously published articles in the series, visit https://www.consultant360.com/specialty/Dermatologic-Disorders/Photo-Essay
Pernio (Chilblains)
Pernio, also referred to as chilblains, is a localized inflammatory eruption of the skin characterized by painful and/or pruritic, erythematous, or violaceous skin lesions most often affecting the distal extremities.1 Primary (idiopathic) pernio, the most common form of pernio, typically occurs after prolonged exposure of non-adapted tissue to cold, non-freezing cold temperatures.2,3
The peak incidence of primary pernio is between 15 and 30 years of age, although individuals in any age group can be affected.4,5 There is a female predominance,4-6 but the most common trigger is exposure to cold, damp, and nonfreezing conditions. Primary pernio occurs more commonly in individuals wearing cold wet shoes or boots or walking in bare feet, especially in the winter months.2,3
The exact pathogenesis of pernio is not known. Primary pernio is believed to be due to vasospasm leading to local hypoxemia and a subsequent secondary inflammatory reaction.3,7 Secondary pernio, which accounts for less than 7% of all pernio cases, is usually associated with systemic lupus erythematosus (chilblain lupus erythematosus, which is the most common), rheumatic arthritis, Behcet disease, antiphospholipid syndrome, monoclonal gammopathy, cryoglobulinemia, celiac disease, chronic myelomonocytic leukemia, blast crisis in acute lymphoblastic leukemia, and Aicardi-Goutières syndrome.3-5,8-11 There is emerging evidence that pernio and pernio-like skin lesions are associated with COVID-19.12-17 In this regard, a high prevalence of cryofibrinogenemia has been detected in patients with pernio during the COVID-19 pandemic.12
Primary pernio usually develops 12 to 24 hours after exposure to the cold.4,5,10 Typical symptoms include pruritus, burning, or intense pain in the affected area.1,5 Characteristically, pernio presents as symmetric, erythematous to violaceous, edematous macules, papules, nodules or plaques (Figures 1 to 3).2
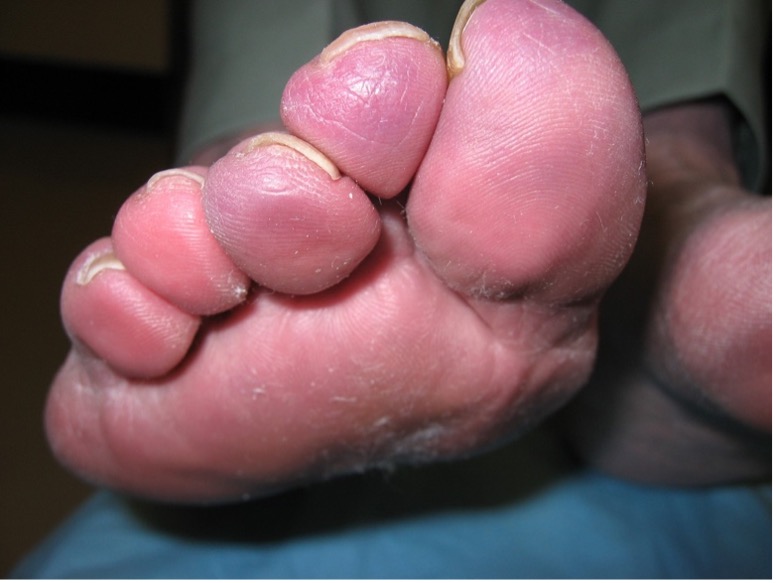
Figure 1. Primary pernio usually develops 12 to 24 hours after exposure to the cold.

Figure 2. Pernio presents as symmetric, erythematous to violaceous, edematous macules, papules, nodules or plaques.

Figure 3. Toes and fingers are most commonly affected by pernio.
In severe cases, vesicles, blisters, erosions, and ulcers may be observed.2,3,18 Toes and fingers are the sites of predilection, although ears, nose, heels, and thighs may also be affected.1,3,6
The overall prognosis of primary pernio is good as lesions tend to resolve within a few weeks.7,10 Complications include tissue necrosis if vasospasm is prolonged, secondary infection, and nail dystrophy.7 In patients who develop pernio secondary to an underlying disease, the prognosis depends on the underlying condition and how well it is controlled.
The diagnosis of primary pernio is mainly clinical, based on a history of exposure to cold, subsequent improvement of symptoms with removal of cold exposure, and the characteristic skin lesions. For secondary pernio, clinical features of the underlying disease should give a clue to the diagnosis.
1. Chan Y, Tang WY, Lam WY, Loo S, Li S, Au A, et al. A cluster of chilblains in Hong Kong. Hong Kong Med J. 2008;14:185-191.
2. Brown PJ, Zirwas MJ, English JC III. The purple digit: an algorithmic approach to diagnosis. Am J Clin Dermatol. 2010;11(2):103-116. doi:10.2165/11530180-000000000-00000.
3. Gordon R, Arikian AM, Pakula AS. Chilblains in Southern California: two case reports and a review of the literature. J Med Case Rep. 2014;8:381. doi:10.1186/1752-1947-8-381.
4. Parra SL, Wisco OJ. What is your diagnosis? Perniosis (chilblain). Cutis. 2009;84(1):27-29.
5. Simon TD, Soep JB, Hollister JG. Pernio in pediatrics. Pediatrics. 2005;116(3):e472-e475. doi:10.1542/peds.2004-2681.
6. Külcü Cakmak S, Gönül M, Oğuz ID, Yayla D, Gül U, Köse K. Demographical, laboratory and associated findings in patients with perniosis. J Eur Acad Dermatol Venereol. 2014;28(7):891-894. doi:10.1111/jdv.12199.
7. Whitman PA, Crane JS. Pernio. StatPearls Publishing; 2020.
8. Lemieux A, Sanchez Vivas NE, Powell J, Jantchou P, Morin MP. Pernio as the clinical presentation of celiac disease: A case report. SAGE Open Med Case Rep. 2020;8:2050313X20940442. doi:10.1177/2050313X20940442.
9. Park KK, Tayebi B, Uihlein L, Speiser J, Mir A, Gerami P, et al. Pernio as the presenting sign of blast crisis in acute lymphoblastic leukemia. Pediatr Dermatol. 2018;35(1):e74-e75. doi:10.1111/pde.13366.
10. Vano-Galvan S, Martorell A. Chilblains. CMAJ. 2012;184(1):67. doi:10.1503/cmaj.110100.
11. Yarbrough K, Danko C, Krol A, Zonana J, Leitenberger S. The importance of chilblains as a diagnostic clue for mild Aicardi-Goutieres syndrome. Am J Med Genet A. 2016;170(12):3308-3312. doi:10.1002/ajmg.a.37944.
12. Gómez-Fernández C, López-Sundh AE, González-Vela C, Ocejo-Vinyals JG, Mayor-Ibarguren A, Salas-Venero CA, et al. High prevalence of cryofibrinogenemia in patients with chilblains during the COVID-19 outbreak. Int J Dermatol. 2020;59(12):1475-1484. doi:10.1111/ijd.15234.
13. Ladha MA, Dupuis EC. SARS-CoV-2-related chilblains. CMAJ. 2020;192(28):E804. doi:10.1503/cmaj.201348.
14. Massey PR, Jones KM. Going viral: A brief history of Chilblain-like skin lesions ("COVID toes") amidst the COVID-19 pandemic. Semin Oncol. 2020;47(5):330-334. doi:10.1053/j.seminoncol.2020.05.012.
15. Mohan V, Lind R. Chilblains in COVID-19 infection. Cureus. 2020;12(7):e9245. doi:10.7759/cureus.9245.
16. Rubin A, Alamgir M, Rubin J, Rao BK. Chilblain-like lesions with prominent bullae in a patient with COVID-19. BMJ Case Rep. 2020;13(11):e237917. doi:10.1136/bcr-2020-237917.
17. Zaladonis A, Huang S, Hsu S. COVID toes or pernio? Clin Dermatol. 2020;38(6):764-767. doi:10.1016/j.clindermatol.2020.06.002.
18. Takci Z, Vahaboglu G, Eksioglu H. Epidemiological patterns of perniosis, and its association with systemic disorder. Clin Exp Dermatol. 2012;37(8):844-849. doi:10.1111/j.1365-2230.2012.04435.x.


