Peer Reviewed
Diagnostic Challenges of Psoriasis: A Multifaceted Case of Triple-Drug Interaction and Literature Review
A 37-year-old woman presented to her primary care physician with erythematous and pruritic patchy lesions on her scalp that had been present for a year, which the patient initially presumed to be associated with dandruff and seborrheic dermatitis. Despite managing symptoms with moisturization, the condition persisted.
History. Upon consultation with a primary care physician, a diagnosis of fungal scalp infection was made based on clinical findings, leading to the initiation of daily terbinafine 250 mg. However, 3 days post-initiation, the patient presented with a broad plaque-like rash on her trunk and lower extremities (Figure 1), prompting hospitalization.
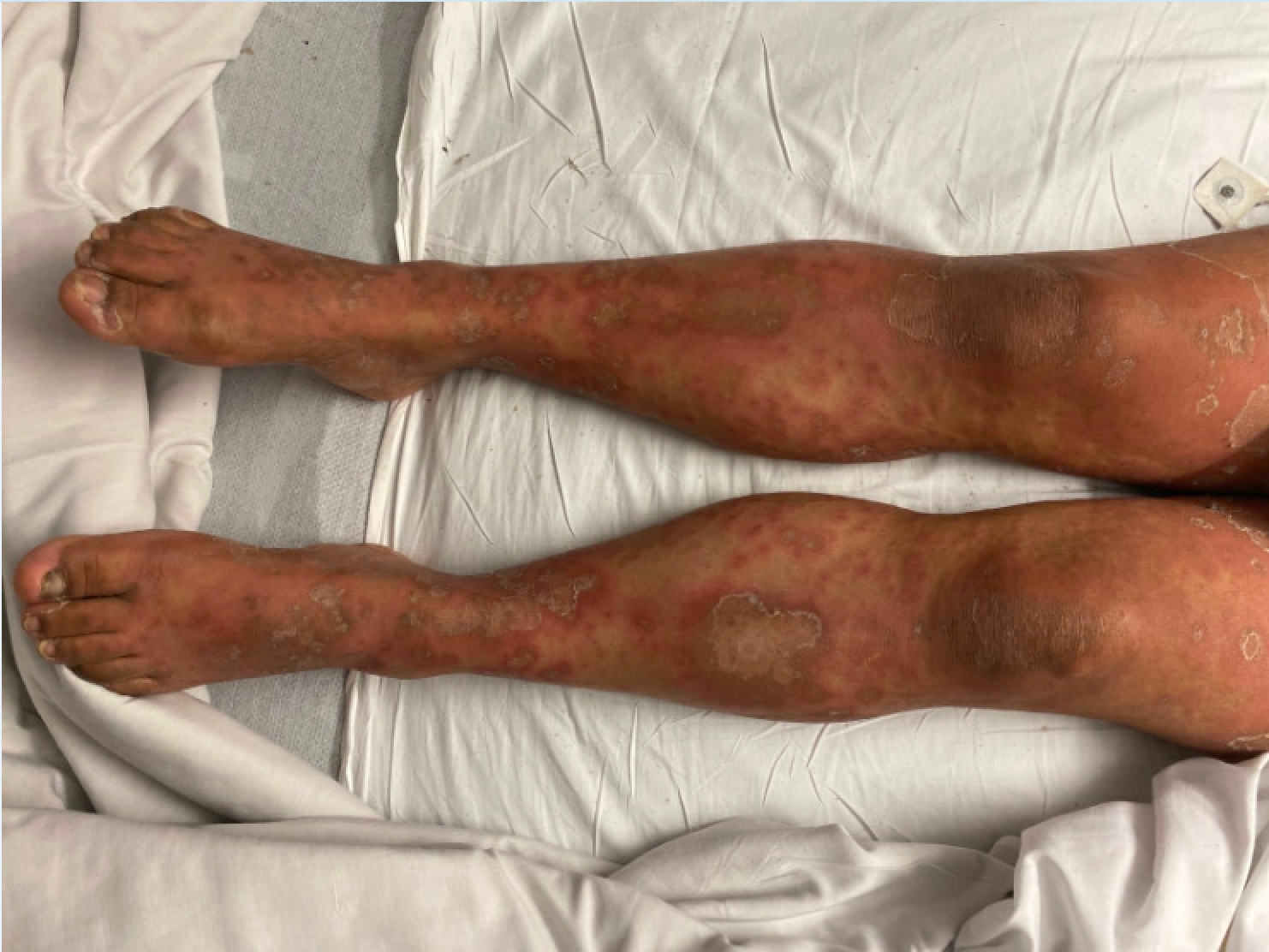
Figure 1. Lower extremity erythroderma in the patient upon hospitalization.
The physical examination was unremarkable aside from the dermatologic findings. The patient denied recent weight changes, joint pain, abdominal pain, nausea, vomiting, and heat or cold intolerance.
Diagnostic testing. A potassium hydroxide (KOH) preparation test was negative. The initial diagnosis was drug-induced cutaneous lupus erythematosus based on the patient’s age, gender, and symptoms. Treatment with prednisone 40 mg and hydroxychloroquine 200 mg was initiated.
Subsequent rapid progression of erythroderma led to further evaluation. Despite an unremarkable complete blood count, basic metabolic panel, and negative infectious panel, the patient was positive for antinuclear antibody, ribonucleotide antibody, and CD50. Skin biopsy findings supported the diagnosis of drug-exacerbated psoriasis, demonstrating characteristic features such as epidermal hyperplasia, parakeratosis, and inflammatory infiltrate predominantly composed of lymphocytes and neutrophils.
Differential diagnoses. Distinguishing among psoriasis, fungal scalp infections, drug-induced cutaneous lupus erythematosus, and other dermatological conditions requires a comprehensive evaluation considering various clinical, laboratory, and histopathological features.
Autoimmune psoriasis typically manifests as well-demarcated erythematous plaques with silvery scales, commonly involving extensor surfaces, nails, and the scalp. Diagnostic criteria encompass the presence of characteristic skin lesions, nail changes, and histopathological findings such as Munro microabscesses and elongation of rete ridges.1
In contrast, fungal scalp infections present with scaling, erythema, and occasionally pustules, necessitating confirmation via microscopy or fungal culture of skin scrapings. A fungal scalp infection was ultimately ruled out by the negative KOH preparation test.
Drug-induced cutaneous lupus erythematosus may present with annular or papulosquamous lesions, often sparing the face, accompanied by positive serological markers such as antinuclear antibodies and anti-dsDNA antibodies.2 Distinguishing features include histopathological findings of interface dermatitis and a positive lupus band test on direct immunofluorescence.2 This diagnosis was excluded here due to negative laboratory tests.
Additionally, consideration should be given to alternative dermatological conditions such as eczema, seborrheic dermatitis, and lichen planus, each requiring specific diagnostic criteria for differentiation. Furthermore, contact dermatitis (whether allergic or irritant) can mimic drug-exacerbated psoriasis and necessitates exploration of environmental exposures for an accurate diagnosis. Conditions like pityriasis rosea should also be considered and evaluated based on clinical presentation, laboratory tests, and skin biopsies. Attention to the possibility of reactive arthritis or cutaneous T-cell lymphoma is essential in the differential diagnosis to ensure appropriate therapeutic interventions are tailored to the specific underlying cause. Other conditions to consider include dermatophytosis, pityriasis rubra pilaris, erythema multiforme, and autoimmune blistering diseases such as pemphigus and bullous pemphigoid, each presenting with distinct clinical features and requiring specific diagnostic approaches for accurate differentiation.
Treatment and management. In addition to discontinuing the offending agents (hydroxychloroquine, terbinafine, and corticosteroids in this case), treatment of drug-exacerbated psoriasis may involve the use of monoclonal antibodies targeting specific cytokines implicated in psoriasis pathogenesis, such as anti-tumor necrosis factor agents or anti-interleukin-17 agents.3 Other potential treatment options include topical corticosteroids, calcineurin inhibitors, and phototherapy.3 In this case, monthly injections of secukinumab 300 mg, an anti-interleukin-17 monoclonal antibody, led to symptom improvement.
Outcome and follow-up. A year post-rash emergence, spontaneous regression of lesions was observed with mild hyperpigmentation. The patient remains stable to date.
Discussion. This case illuminates the intricate challenges associated with diagnosing psoriasis, revealing a situation of mismanagement. Terbinafine, an antifungal medication, has been implicated in potentially worsening psoriasis through hypothesized immunomodulatory effects and genetic factors, heightening the immune response linked to psoriatic lesions.4 The intricate interplay between terbinafine, the immune system, and genetics underscores the complexity of drug-induced exacerbations in psoriasis. Hydroxychloroquine, an antimalarial drug, has been associated with potential psoriasis exacerbation by modulating the immune system and disrupting cytokine balance.5 The nuanced interactions within the immune system and the variable individual responses to hydroxychloroquine underscore the necessity for careful consideration and monitoring of patients when prescribing this medication. Moreover, abrupt steroid withdrawal can induce ‘rebound psoriasis,’ characterized by the prompt recurrence or worsening of psoriatic symptoms.5,6 The immunosuppressive effects of systemic corticosteroids necessitate gradual tapering to avoid unintended flare-ups, highlighting the importance of meticulous steroid withdrawal management for long-term psoriasis control.
While prior studies have individually explored the association between each drug and psoriasis, the novelty of this case lies in its presentation of triple-drug-exacerbated psoriasis.4-6 The convergence of terbinafine, hydroxychloroquine, and systemic corticosteroids in a single case resulting in exacerbated psoriasis contributes a unique layer to the existing literature, emphasizing the cumulative impact of these medications on psoriatic manifestations, creating a complex and challenging clinical scenario.
This case highlights the need to recognize and address the combined effects of multiple drugs in patients with psoriasis, emphasizing the need for heightened vigilance and a nuanced approach in complex therapeutic scenarios. Moreover, it sheds light on the intricacies of diagnosing psoriasis, particularly in medication-related exacerbations. The initial misdiagnoses of both a fungal scalp infection and drug-induced cutaneous lupus erythematosus, followed by the subsequent development of rapidly progressive erythroderma, highlights the challenges in distinguishing between various skin conditions, especially when medication-induced effects are in play.6 The complexity arises from the overlapping clinical presentations of different dermatological disorders and the potential for drugs like terbinafine and hydroxychloroquine to mimic or exacerbate psoriasis.
This case emphasizes the critical need for a comprehensive, interdisciplinary approach to diagnosing and managing psoriasis. In clinical practice, health care professionals, primarily dermatologists, must exercise heightened awareness when prescribing medications that may interact with psoriasis or trigger its exacerbation. A thorough evaluation, including skin biopsies and collaboration between dermatologists and other relevant specialties such as rheumatologists, is essential for accurate diagnosis, particularly when faced with atypical presentations or adverse drug reactions. This case emphasizes the evolving landscape of psoriasis treatment, exemplified by the successful management of the patient with monoclonal antibody injections. This underscores the importance of staying informed about advancements in psoriasis therapies and tailoring treatment strategies based on each patient's specific characteristics and triggers.4
Overall, the case serves as a reminder of the dynamic nature of psoriasis diagnosis and treatment, emphasizing the ongoing need for education and collaboration among health care professionals to ensure optimal patient care. Identifying medication-related exacerbations and induction of psoriasis in clinical practice can be challenging, making the recognition of potential drug-related psoriasis clinically relevant for optimal management.
- Bhuntani T, Liao W, Nakamura M. Updates in Clinical Dermatology. Springer; 2018. Accessed June 5, 2024. doi:10.1007/978-3-319-90107-7_1.
- Solhjoo M, Goyal A, Chauhan K. Drug-Induced Lupus Erythematosus. StatPearls Publishinng, April 2, 2023. Accessed June 5, 2024. https://www.ncbi.nlm.nih.gov/books/NBK441889/
- Bakshi H, Nagpal M, Singh M, Dhingra GA, Aggarwal G. Treatment of psoriasis: a comprehensive review of entire therapies. Curr Drug Saf. 2020;15(2):82-104. doi:10.2174/1574886315666200128095958.
- Zaouak A, Chamli A, Koubaa W, Hammami H, Fenniche S. Generalized pustular psoriasis induced by terbinafine. Presse Med. 2019;48(9):1009-1011. doi:10.1016/j.lpm.2019.07.006.
- Wang WM, Wang KY, Wang T, Jin HZ, Fang K. Hydroxychloroquine-induced psoriasis-form erythroderma in a patient with systemic lupus erythematosus. Chin Med J (Engl). 2018;131(15):1887-1888. doi:10.4103/0366-6999.237411.
- Long V, Yew YW, Chandran NS, Choi EC. Psoriasis flares and rebound phenomenon following exposure and withdrawal of systemic steroids: a systematic review and meta-analysis. J Am Acad Dermatol. 2022;87(3):660-661. doi:10.1016/j.jaad.2022.01.006.
AFFILIATION:
University of Arizona College of Medicine – Phoenix, Phoenix, AZ
CITATION:
Shah D. Diagnostic challenges of psoriasis: a multifaceted case of triple-drug interaction and literature review. Consultant. 2024;64(6):e3. doi:10.25270/con.2024.06.000002
Received December 12, 2023. Accepted April 8, 2024. Published online June 10, 2024.
DISCLOSURES:
The authors report no relevant financial relationships.
ACKNOWLEDGEMENTS:
None.
CORRESPONDENCE:
Divya Shah, MD, 6735 E Greenway Parkway Apt 2117, Scottsdale, AZ 85254 (shahdivya28@gmail.com)


